-
Physiotherapy

Physiotherapy is an independent self-regulated profession, encompassing a broad range of services. Physiotherapists are primary health care professionals that are responsible for assessment, diagnosis and treatment of a variety of medical conditions. They combine their in-depth knowledge of the body and how it works and translate it to customized treatments to maximize outcomes for each and every illness, injury, and disability.
Physiotherapy assessments and subsequent treatments will focus primarily on an orthopedic caseload but will not be limited to other aspects of physiotherapy. The following will be offered through our physiotherapy services:
- Acute Injury Management
Acute care management of all sprains and strains (i.e. sprained ankle, strained hamstring) will be available. Treatment may include a combination of education, protective bracing, bandaging and splinting, anti-inflammatory electrical modalities such as ultrasound, laser, or interferential current, application of ice, and manual therapy if indicated to minimize pain and swelling, and implementation of an exercise program when appropriate. - Sports Related Injuries
Rehabilitation of sports related injuries is designed to facilitate a timely and appropriate return to pre-injury function. Rehab will consist of sport specific exercises to maximize strength and mobility restrictions, improve flexibility, coordination and balance to achieve peak athletic performance while reducing the susceptibility and reoccurrence of future injuries. - Repetitive Sprain and Strain Injuries
Repetitive sprain and strains injuries differ from acute injuries in that they are more chronic in nature. Treatment for these injuries will benefit from further education, activity modifications, gentle exercise, specific and focused strengthening, potential use of bracing or splinting with a gradual return to activity. - Pre and Post Surgical Rehabilitation
Tailored programs including exercise and education will be offered to patient’s pre and post surgery to maximize outcomes post surgery. Skilled physiotherapist’s will be knowledgeable in protocols for each procedure and modify exercises as necessary to aid in the most favorable treatment for each patient. Communication with the surgeon will be vital for optimal recovery, which the physiotherapist will take part in throughout the patient’s rehab. - Manual and Manipulative Therapy
Manual and manipulative therapy involves the use of a physiotherapist’s hands to clinically manipulate and mobilize soft tissue and joints. This may include therapist-assisted stretches, articular mobilizations and manipulations, local soft tissue massage, friction massage, myofascial release and acupressure. Manipulations are passive, high velocity, low amplitude thrusts applied to a joint beyond its physiological limit of motion, but within its anatomic limit with the intent to restore optimal motion, function and reduce pain. - Customized Exercise Programs
An important component of any physiotherapy program is the implementation of a customized and individualized exercise program. Components of the exercise program are transferable to a home setting for improved adherence as well as efficacy. Physiotherapist assisted stretching, postural re-education techniques, resisted training, cardiovascular conditioning and implementation of changes acquired through education will be components of the program. Strengthening equipment will be available at the clinic specific to rehabilitation which may include but are not limited to an upper body cycle, a recumbent bike, treadmill, a universal machine, theraband resisted tubing, wall mounted resisted pulleys and therapy balls. - Taping and Strapping
Protective taping, tensoring and bandaging services and supplies are available for protection, stabilization and support of injured joints and soft tissue. Application is suitable in all stages of injury, acute and chronic. - Electrotherapeutic Modalities and Thermotherapy
Various modalities including ultrasound, laser, multi-current stimulation including interferential current (IFC), transcutaneous nerve stimulation (TENS) and electrical neuro-muscular stimulation (NMES) are utilized in the treatment of pain, swelling and muscular weakness. The clinic will be well equipped with an assortment of electrical stimulation modalities available as part of a treatment program. - Mechanical Traction
A mechanical traction unit will provide the ability to longitudinally stretch the neck and low back. A modernized unit will be in place with patient specific programming and protocols. The technique is utilized for the treatment of spinal conditions including disc protrusions, degenerative disc disease and spinal arthritis.
- Acute Injury Management
-
Massage Therapy
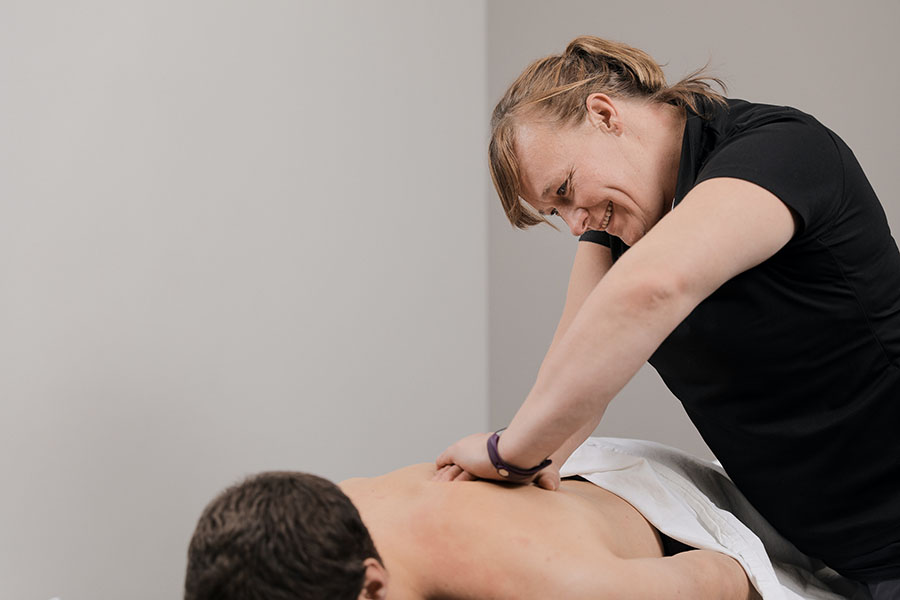
Massage therapy will be offered by Complete Physiotherapy in conjunction with the physiotherapy and above-mentioned services. Services will be therapeutic in nature for the treatment of both orthopedic disorders and relaxation.
Licensed massage therapists are extensively trained in the safe application of manual mobilization of soft tissue and offer a variety of services including pre and post natal, sport massage, lymphatic drainage, relaxation massage, trigger point and myofascial techniques.
-
Athletic Therapy
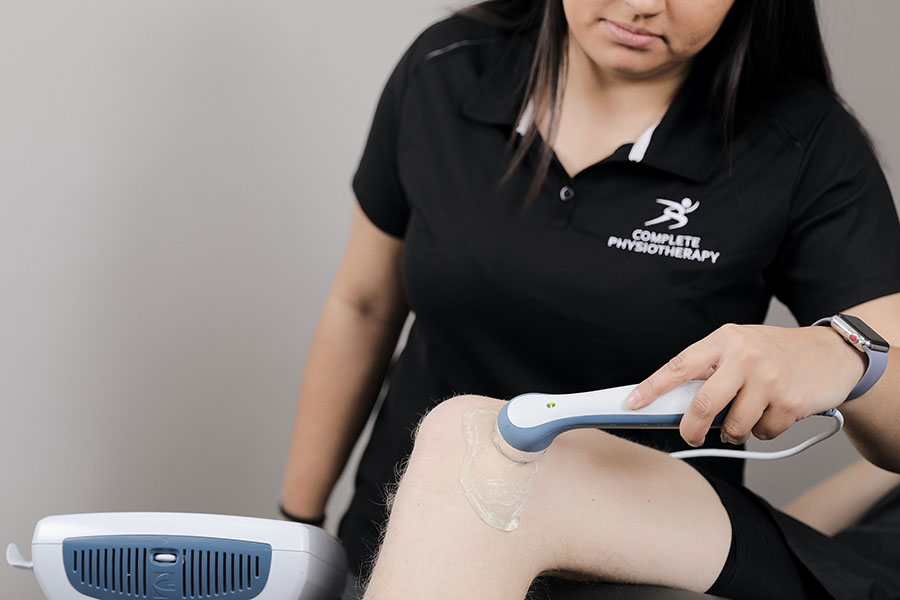
Athletic Therapy is the assessment and treatment of musculoskeletal injuries both in a clinical setting and on the sidelines of sporting events. Treating patients with acute and chronic muscle, bone and joint injuries, a Certified Athletic Therapist can help you recover from a sprain, strain, fracture or joint replacement surgery.
Athletic Therapists use the Sports Medicine Model of Care:
- Prevention
- Assessment
- Treatment
- Rehabilitation
- Education
Treating a wide range of clients from children to seniors, a Certified Athletic Therapist works to help you return back to your daily activities, whether that means playing competitive or recreational sport, returning to work, or being able to play with your grandchildren. Using manual techniques, modalities, exercise, taping and patient education, an Athletic Therapist works to get you back to doing the things you love to do.
-
Vestibular Rehabilitation (Dizziness, Vertigo and Balance Rehabilitation)

Dizziness and vertigo are among the most common symptoms that send people to see doctors. Many of these vertigo and dizziness problems come from a dysfunction of the inner ear or the vestibular organ. The vestibular organ is critical for balance, coordination, and movement, and when it is in dysfunction patients can experience spinning (vertigo), dizziness, visual disturbances, nausea, imbalance, and light-headedness.
Vestibular rehabilitation is a form of therapy intended to alleviate both the primary and secondary problems caused by vestibular disorders. Evidence has shown that vestibular rehabilitation can be effective in improving symptoms related to many vestibular (inner ear/balance) disorders.
Conditions commonly treated or helped with vestibular rehabilitation include:
- Benign Paroxysmal Positional Vertigo (BPPV/Vertigo)
- Unilateral or Bilateral Hypovestibular Disorders caused by:
- Vestibular Neuritis
- Labyrinthitis
- Meniere’s Disease
- Acoustic Neuroma
- Central Causes of Vestibular Dysfunction
- Stroke
- Acquired Brain Injuries/Concussions
- Tumours (after surgery)
- Vestibular Migraines
Once a diagnosis has been determined by your physiotherapist, an individualized rehab program will be created for you that may involve repositioning techniques of the crystals in the inner ear, gaze stabilization exercises, motion sensitivity exercises or habituation exercises, and balance and coordination exercise.
-
Post Concussion Management

Concussions are forms of brain injury resulting from a direct or indirect blow to the head, face or jaw causing an alteration in brain function. As concussions produce a wide array of symptoms, this can pose a challenge to coaches, trainers, parents and health professionals involved in the care of the injured athlete.
The time frame for recovery varies widely for every patient, making it that much more imperative to have specific and tailored rehab programs for every individual that presents with concussion-like symptoms to reduce the risk of premature sport activity and delay full return to pre-injury levels.
Key components of concussion treatment include education, prevention and management emphasizing individualized resting strategies, specific recommendations regarding return to work and play, manual therapy for associated neck complaints, screening and referral for vision therapy, balance, coordination and vestibular-based rehabilitation and tailored exercise plans for return-to-sport. All these services are offered and accessible through the physiotherapy clinic.
-
Temporomandibular (Jaw) Joint Treatment

The temporomandibular joint, or TMJ is the joint that connects your jawbone to your skull. There are many causes of temporomandibular dysfunction (TMD) including arthritis, jaw injury or clenching and teeth grinding. Physiotherapists can assess, diagnose, treat and refer those individuals presenting with TMD to other health care professionals including dentists and physicians.
Treating the TMJ is a unique area of practice that requires a more personal relationship with the therapist as it involves the physiotherapists gloved hand in the patient’s mouth to accurately assess, diagnose and treat the injury.
-
Hand and Upper Extremity Therapy

Hand and Upper Extremity Therapy is a unique area of practice that involves rehabilitation of the upper limb, including the hand, wrist, elbow and shoulder girdle. It is a merging of occupational and physical therapy theory and practice that combines comprehensive knowledge of the structure of the upper limb with function and activity. Using specific skills in assessment, diagnosing, planning and treatment, physiotherapists provide evidenced based, therapeutic interventions to prevent long lasting dysfunction, restore function, maximize outcomes and restore quality of life.
Treatment for the upper extremity may include bracing and splinting, post-surgical rehabilitation, manual therapy, graded motor imagery, sensory re-education, scar and swelling management.
-
Pelvic Floor Physiotherapy
The Pelvic floor is a commonly overlooked group of muscles in the body. These muscles and ligaments run from the pubic bone to tailbone to the sit bones and across. The pelvic floor performs a large roll in stabilization, continence and can be a source of pain for 1 in 5 people. Pelvic floor dysfunction can develop from either tight, weak, or poorly coordinated muscles. Pelvic floor treatment is available to women, men, and children of all ages. Through an extensive hands-on examination, a pelvic floor therapist can determine one’s source of dysfunction in order to improve upon their symptoms.
Commonly Treated Conditions:
- Bladder and Bowel Incontinence
- Overactive Bladder
- Constipation
- Pelvic Pains
- Sexual Dysfunctions/Pains
- Pelvic Organ Prolapse
- Abdominal Pains Associated with Bloat
- Low Back, Hip or Coccyx (Tailbone) Pains
- Athletes
- Pre and Post Operative Surgeries
What To Expect:
A pelvic floor therapist will take an extensive history detailing one’s dysfunctions, pains, goals, and past medical history. From there, the therapist will perform a movement-based assessment, and external examination of the pelvic floor region. With approval, the therapist will also perform an internal pelvic exam using gloves and lubricant, looking for sources that could be contributing to the cause of dysfunction. Once this is completed, the therapist will provide treatment for the dysfunctions found. In addition, patients can expect education and prescribed exercises to help facilitate the improvement of their condition.
-
Reconditioning and Work Hardening Programs

Specific reconditioning and return to work programs are designed for patients injured in motor vehicle accidents (MVA), workplace injuries, or have suffered significant trauma and psychological stresses. These programs are meant to facilitate a gradual return to work and best prepare and accustom the patients injured body to their previous work duties while decreasing the chance of further musculoskeletal injuries.
A Kinesiologist/Personal Trainer may be involved throughout the program to provide one on one patient care to ensure exercises are being completed safely, in a timely fashion and as prescribed. The physiotherapist will oversee the program and administer a detailed initial, mid-term and final assessment with reports encompassing the detailed assessment to be sent to the case managers for the 3rd party insurers.
In addition to the reconditioning/work hardening programs, Complete will also include detailed education on pain mechanisms, pain management, and provide the patients with various resources to help maximize their progress within the program.
-
Acupuncture
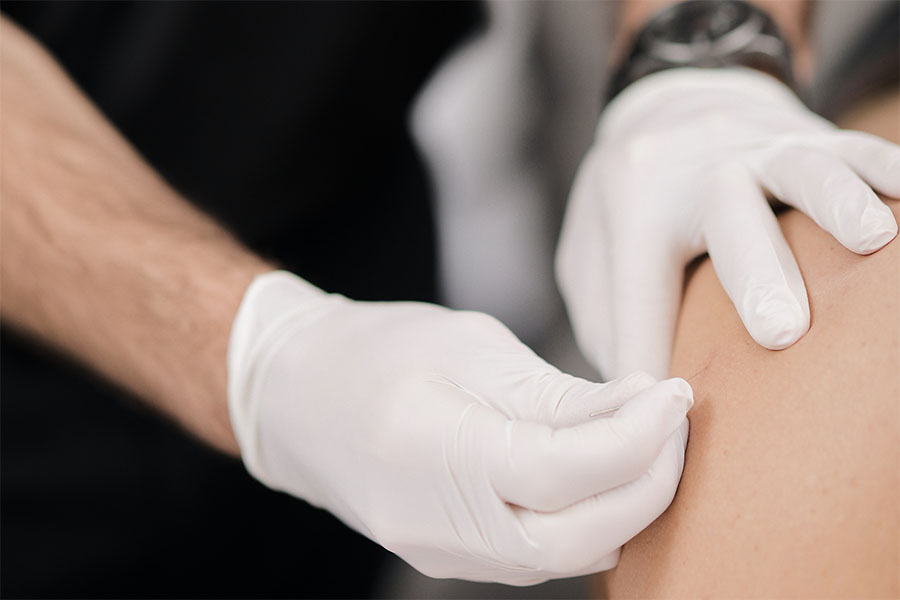
Acupuncture for the modulation of pain may be incorporated into patient treatment regimes. It is designed to treat both the symptoms and the root cause of the patient’s injury or illness. It is a safe and effective treatment option that stimulates the release of endorphins facilitating pain relief, increasing energy, improving overall mood and body function.
Due to extensive post-graduate training and examinations being required to safely practice acupuncture in Manitoba, only those physiotherapists who have completed the above requirements are able to and will administer this treatment to patients.
-
Dry Needling

Dry Needling, what is it and how does it work?
Dry needling is a technique used in which a fine sterile filiform needle is used to penetrate the skin and muscle for the treatment of pain and movement impairments. These needles contain no liquid, and nothing is injected. It is an effective treatment for acute and chronic pain.
Physiotherapists practice dry needling with the primary goal of releasing or inactivating trigger points to relive pain or improve range of motion. During treatment it is common to feel or experience a local twitch response of the target tissue. This is the first step in breaking the pain cycle which will improve flexibility and decrease pain. This may help speed up the patients return to active rehabilitation and function.
Sometimes we add electrical stimulation to the solid filiform needles during a dry needling session. Electro-stimulation improves the circulation of natural analgesics (endorphins and opioids) in order to reduce pain. Blood circulation is also stimulated, promoting the delivery of nutrients to tissue, speeding up the healing processes. Electro-stimulation allows stronger, more continuous stimulation. The Electro-stimulation treatment lasts approximately 10-15 minutes and you will be free to go about your usual activities post treatment.
What types of conditions can dry needling assist?
- Neck/Back pain
- Shoulder pain
- Tennis/Golfers Elbow
- Hip and Gluteal pain
- Plantar Fasciitis
- Sciatica
- Muscle strains and sprains
- Headaches
-
Custom Foot Orthotics
Detailed biomechanical foot assessments and orthotic prescription will be provided for patients whose injuries and ailments dictate the need for these custom inserts. Orthotics provide accommodation of existing foot deformities, superior motion control and support, biomechanical correction and shock absorption.
A casting technique is used as a mold to fabricate a custom permanent shoe insert. They are lightweight, durable and come in a variety of styles to easily fit most footwear. Complete uses Paris Orthotics based out of Vancouver as the provider for all orthotics.
-
Personal Training
You don’t need an injury to come to the clinic. Join us to get stronger, healthier and more confident.
Proper exercise prescription helps improve body composition, physical performance, heart condition and health outcomes. Our trainers possess the knowledge, skills and abilities necessary to design safe and effective fitness programs. We instruct and assist people in reaching their personal health and fitness goals. Our trainers deliver safe, effective, fun and interesting workouts to all clients. The training programs are varied and progressive, and geared toward improving clients’ health and wellness.
Individual or small group training is available.
-
Titleist Performance Golf Provider
The Titleist Performance Institute (TPI) is the Gold Standard when it comes to health, fitness and performance in Golf. Its philosophy is that “while there are many ways to swing a golf club, there’s one efficient way for each golfer based on their individual physical capabilities”.
Since its inception in 2003, TPI has helped thousands of golfers, ranging from a beginner golfer, to some of the best in the world. Certified TPI professionals include personal trainers, coaches and health care professionals, with each avenue dedicated to help golfers in different ways.
If you are looking to recover from a golf injury, or looking to be able to play golf pain free, our Level 3 certified physiotherapist will be able to help you. The mission at TPI is to educate golfers about their Body-Swing Connection, which helps identify the body’s limitations, whether it is mobility or stability. They will start with a comprehensive exam that will help identify the root cause of your pain followed by a treatment plan to help get you back on the course.
Most Common Golf Injuries:
- Sprain/Strain
- Tendinitis
- Arthritis
- Disc Injuries
- Tears/Fractures
Most Common Mechanism of Golf Injuries:
- Poor Body Mechanics
- Poor Swing Biomechanics
- Excessive Practice (Overuse)
- No regular Customized Exercise Program
- Poor Nutrition
- Improper Club Fitting
